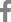INTRODUCTION
Musculoskeletal involvements, including the joints, tendons, muscles, cartilage, and even bones, are not uncommon clinical manifestations in systemic lupus erythematosus (SLE) [1]. However, enthesopathy or enthesitis have not been reported in patients with SLE. Enthesitis, which is characterized by inflammation at the point of insertion of a ligament, tendon, or joint capsule to bone, has traditionally been regarded as a hallmark of spondyloarthropathies (SpA), especially ankylosing spondylitis (AS) [2].
Here, we present the first case of enthesitis in a patient with SLE and antiphospholipid syndrome (APS).
CASE REPORT
A 36-year-old woman with SLE presented to the rheumatology clinic with low back pain showing a gradual increase in intensity for 4 months. She had been diagnosed with SLE 6 years previously, manifested by WHO class III lupus nephritis, autoimmune hemolytic anemia, thrombocytopenia, hypocomplementemia, and positive anti-nuclear and anti-double-stranded DNA antibodies. Furthermore, she had a history of middle cerebral artery infarction 1 year later due to APS. A diagnosis of APS was previously established on the basis of a history of recurrent spontaneous abortions (more than three times), positive lupus anticoagulant, positive anti-cardiolipin antibodies, and false-positive VDRL. Despite these previous complications, her SLE and APS were under reasonably good control with medications, including prednisone (5 mg daily), hydroxychloroquine (200 mg twice daily), and enoxaparin (40 mg/day) at the time of presentation. Warfarin had been switched to enoxaparin 3 years ago due to her desire to be come pregnant. She reported no previous history of trauma to her back, but stated that morning stiffness was present.
Upon physical examination, the patient was afebrile, and vital signs were normal. There was no limitation in range of motion of the lumbar spine. Point tenderness around the lower lumbar spine was noted. The complete blood cell count was normal. The erythrocyte sedimentation rate and C-reactive protein level were slightly elevated at 48 mm/h (normal range 0~22 mm/h) and 0.36 mg/dL (normal range 0~0.3 mg/dL), respectively. Anti-double-stranded DNA antibody level had been stable, and at the time of the clinic visit, it was 16.9 IU/mL (normal range 0~7 IU/mL).
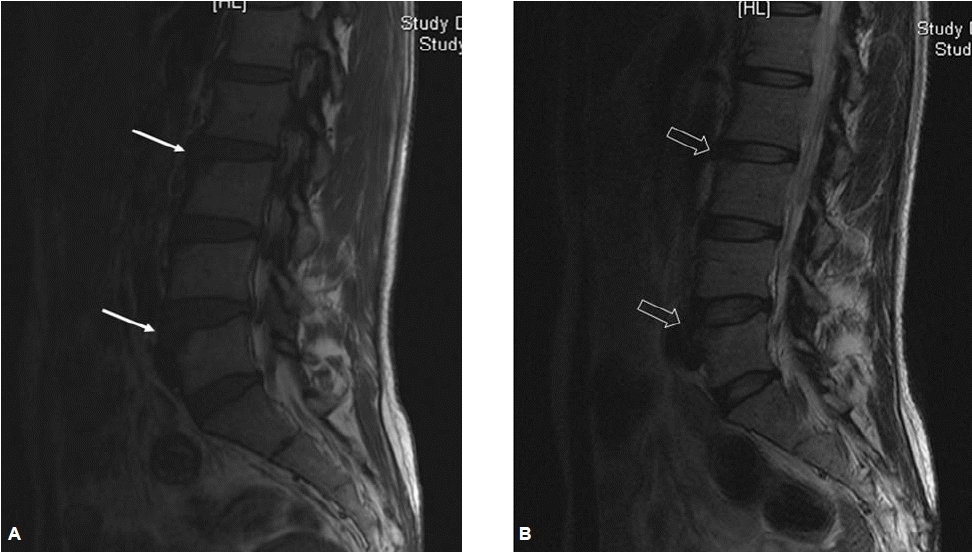
Aradiograph of the lumbar spine revealed sclerosis at the anterior superior bodies of L3 and L5 (Fig. 1). The sacroiliac joints had a normal appearance. Further evaluation included magnetic resonance imaging (MRI) of the lumbar spine, which showed low-intensity signal changes on T1-weighted images and high-intensity signal changes on T2-weighted images at the anterior superior bodies of L3, L4, and L5 (Fig. 2A, 2B). These MRI findings were consistent with osteitis or enthesitis. The initial treatment regimen consisted of a nonsteroidal anti-inflammatory drug (NSAID). Prompt clinical improvement was achieved with resolution of low back pain. A follow-up MRI study 6 months later showed complete resolution of signal changes in the lumbar spine (Fig. 3A, 3B).
DISCUSSION
Musculoskeletal manifestations are commonly encountered in SLE patients and include, but are not limited to, arthritis, tenosynovitis, bursitis, avascular necrosis, and tendon rupture [1]. Furthermore, sacroiliitis, traditionally regarded as a hallmark of SpA, has rarely been reported in SLE patients [3,4]. However, there have been no previous reports of enthesitis or enthesopathy, other pathological changes that are distinctive features of SpA, in patients with SLE. To our knowledge, this is the first report of enthesitis as a musculoskeletal manifestation of SLE.
The radiographic features of enthesitis include soft tissue swelling, osteopenia of subentheseal bone, bone cortex irregularity at the insertion, and adjacent periostitis, as well as entheseal soft tissue calcification and new bone formation. More advanced changes, such as bone sclerosis, erosions, and spurs, may be also detected. On MRI, enthesitis of the spine is characterized by bone edema at the vertebral body or facet articulation. Osteitis (“bone edema”) and enthesitis are part of the same lesion, which many physicians failed to recognize until recently [5,6].
Differential diagnosis of conditions that can cause osteitis of the spine in patients with low back pain includes SpA, as mentioned previously, infections (osteomyelitis, septic discitis, or paravertebral abscess), trauma, degenerative processes, spinal stenosis, diffuse idiopathic skeletal hyperostosis, Paget’s disease, and metastatic lesions [7]. Extensive workup in our patient revealed none of the above underlying diseases.
Human leukocyte antigen (HLA) type, especially HLA-B27 and DR3, has been suggested to play a role in coincidental AS in SLE patients [3,8]. Unfortunately, HLA-B27 serotyping was not performed in this patient. However, the absence of sacroiliitis on MRI excluded the possibility of AS in this case.
The pathophysiology of enthesitis remains largely obscure. Moreover, due to the absence of case reports such as ours and the lack of studies examining this aspect of musculoskeletal manifestations of SLE or the coexisting features of SLE and SpA, the causal mechanism of enthesitis in SLE remains rather speculative and needs to be further elucidated. In AS, on the other hand, the role of CD8+ T cells in the pathogenesis of enthesitis has been investigated, and they may have a key role in driving local inflammation [9].
Conventional NSAID therapy remains the first line of treatment in enthesitis, and local steroid injection can be considered in severe cases.




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print